
No Scalpel Vasectomy
Dr. Engel performs vasectomies in our downtown Washington, D.C. office every Tuesday and does many of these procedures weekly. Dr. Tobon also performs vasectomies in our downtown office. A vasectomy is a straightforward procedure that can be compared to a dental visit. It is done under local anesthesia only; the patient can drive home afterward and does not need any special preparation other than stopping any medicines that may prevent clotting. The procedure itself takes 10-15 minutes. Most patients will feel good enough to go back to work the next day, and since the surgeons at USW perform a no-scalpel vasectomy, there are no stitches in the skin, so there is no need for a follow-up visit a week later.
To explain more about vasectomy in general, let’s first go over some anatomy. The testicles produce sperm, but they do not produce semen. Semen is made by the seminal vesicles, which are located behind the bladder and attach to the prostate. How sperm gets into semen is the key to understanding what a vasectomy is. Sperm is produced in the testicles and then stored in a structure around the top and back of the testicle called the epididymis. Once mature, they travel up a very long pipe (vas deferens) that goes from the epididymis, up the scrotum, into the groin, into the abdomen, loops towards the pelvis, and then plugs in at the prostate and seminal vesicles. So, if one wants to stop sperm from getting to the semen, what needs to be done is to cut the vas coming from each testicle.
The easiest place to get to it is in the scrotum. Thus, a vasectomy is cutting both vasa in the scrotum so one ejaculates semen that has no sperm in it.
A vasectomy will not affect testosterone, erections, or anything other than fertility. There is nothing safer than a vasectomy other than abstinence, but amazingly, there is still a long-term failure rate, and it is essential for all patients to realize this. USW quotes a 0.03% long-term failure rate, and it is stressed that birth control must continue until the patient brings a specimen to their nearest Lab Corp specimen collection center two months after the vasectomy. A patient is not cleared until this specimen is seen on their portal as showing absolutely no sperm. Patients are instructed not to have unprotected intercourse with their partner until they see this result. If there are any questions or any uncertainty about their results whatsoever, we ask that a virtual visit be made with our nurse practitioner right away to discuss and receive instructions.
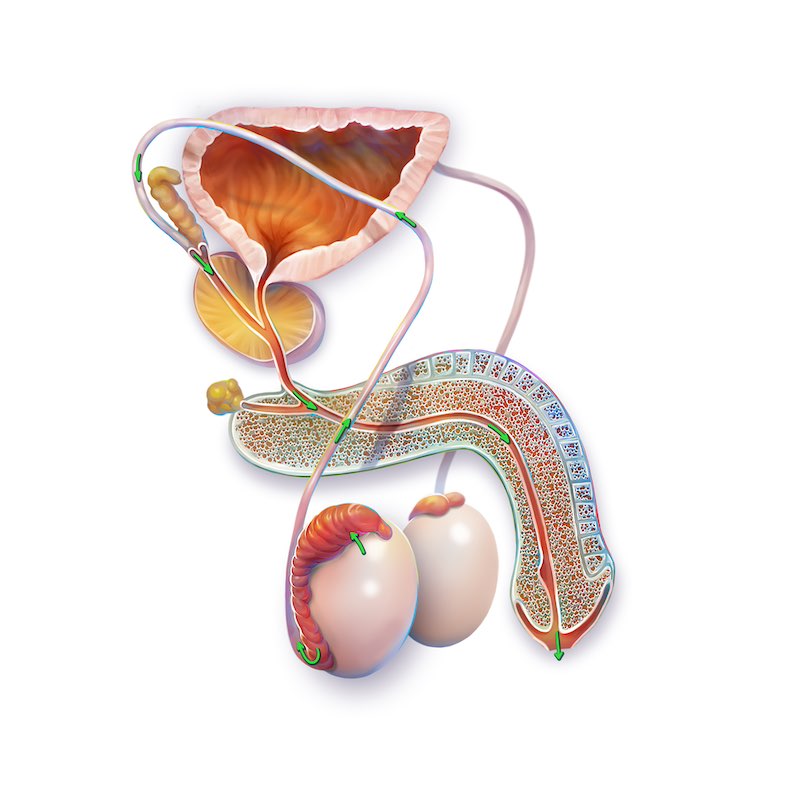
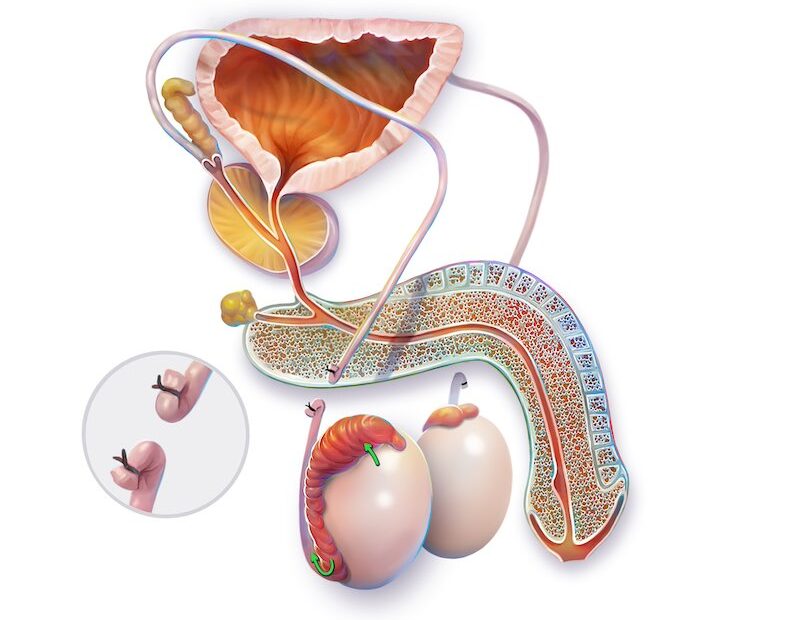
The vasectomy procedure itself is relatively easy and typically not particularly painful. Patients are commonly anxious but almost always are surprised by how easy the process is for them. As with the dentist, first, a shot will be given high in the scrotum on each side. The area will be prepped and draped, and then the patient will be left alone with their phone or a magazine for ten minutes or so to allow the numbing medicine to take full effect. Parts of the vasectomy will be felt, but the pain will not be severe. A puncture is made in the skin, and the vas is elevated up out of the scrotum by feel. No real incision is made. A piece of the vas is removed, the ends cauterized, both ends sewn shut twice, the vas is allowed to fall back into the scrotum, and the puncture site is cauterized. When finished, band-aids only are applied.
After a Vasectomy
The patient is asked to go home for an hour or so. This allows the patient to hold pressure on the two puncture sites with gauze. If done for 30-60 minutes, the complication of bleeding is extremely rare. After that period, applying ice or a bag of frozen peas is optional. No other specific restrictions are given. Patients will exercise or ejaculate as tolerated; we have no specific restrictions other than that baths or swimming are avoided until the wounds are closed. Showering the next day is permitted. There will be soreness for a week or two, along the lines of a jammed finger, that will slowly disappear. Patients are not routinely given pain medicines or antibiotics; pain is managed with ibuprofen afterward, just as dentists do. After a specimen is brought to Lab Corp and shown to have no sperm present two months later, the experience is complete!
We encourage our patients to feel free afterward at any time to have us check them to ensure their recovery is progressing appropriately. We have an open door policy for this in that we ask you to come into the office, no appointment necessary, and have any of us check you at any time.
Vasectomy Risks
Occasionally, the epididymis will get inflamed or swollen due to obstruction. It is not a true infection and will usually only be treated with anti-inflammatory medications. This happens in perhaps 1:200 vasectomies. Infections are exceedingly rare. Other inflammatory responses called sperm granulomas are also infrequent events.
Chronic pain after a vasectomy is controversial and worth noting. This incidence is reported as anywhere from exceedingly rare up to 30% of patients. Realistically, we believe it to be very rare. Chronic pain in the scrotum is a widespread complaint seen by Urologists in patients who have not had vasectomies. In the rare case where a patient is seen many months later who feels as if there is chronic pain from a vasectomy, the presentation is usually identical to those who have not had vasectomies, so it is often unclear what the cause is. It is likewise treated identically. Patients are warned of this at their initial consultation but told that the risk of long-term chronic pain from a vasectomy is very low.
We’d be happy to see you soon to discuss a vasectomy with you and go over any additional questions or concerns you may have.





