Urethroplasty
An urethroplasty is an operation that Dr. Engel performs regularly on his patients when internal urethrotomy fails. As discussed in our section on Urethral Strictures, our initial proposed treatment for urethral strictures is typically direct vision internal urethrotomy (DVIU). Rarely is urethral dilation performed in younger men, as the recurrence rate for this procedure is well above 90%. Internal urethrotomy offers a lower recurrence rate, but even still a stricture will return at least 50% of the time after DVIU for strictures greater than one centimeter.
Stricture Recurrence
When a stricture does recur in a man’s urethra, he will be offered either repeat DVIU or urethroplasty. Sometimes the patient chooses DVIU for scheduling reasons, or sometimes a man is simply not prepared mentally for the larger undertaking of an urethroplasty. However, recurrence rate in the setting of repeat DVIU is probably at least 80%. For this reason, current guidelines at least dictate that in that setting an urethroplasty is at least offered and discussed.
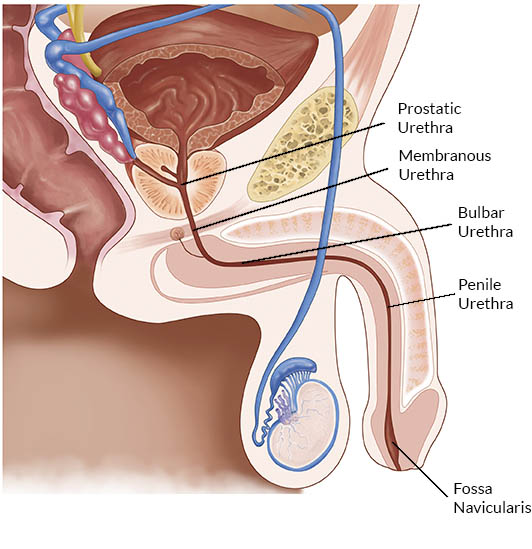
Segments of the male urethra
An urethroplasty is a highly specialized procedure that not all Urologists perform. It is an operation more akin to plastic surgery than other common Urologic procedures, and it is an operation that has evolved tremendously over the last twenty years or so. Most strictures in the male urethra occur in the bulbar urethra, so much of the information below pertains to a bulbar urethroplasty.
If a bulbar urethral stricture is short (less than 1.5 cm) Dr. Engel prefers simply to excise the strictured segment and reconnect the remaining urethral ends. Until buccal mucosa (the lining of one’s cheek) was established as an excellent graft to use for this reconstruction, it was always considered desirable to excise and reconnect strictured urethras in this manner even for much longer strictures. However, once the stricture becomes longer, to excise and reconnect carries the risk of shortening the penis, and in rare circumstances, leading to erectile dysfunction, particularly at the head of the penis or glans. Before buccal mucosa grafts were used, many different flaps and grafts came and went in terms of popularity. Approximately 15 years ago, contemporary thinking favored using penile non-hair bearing skin that was kept alive on its blood supply for reconstruction. Before that, free grafts of skin, some hair bearing, were used. Now, nearly all of these flaps and grafts are no longer used in favor of buccal mucosa, which has simplified greatly the grafting process for urethral reconstruction.
Today, the most common urethroplasty performed is a buccal mucosal onlay onto a bulbar urethra that has been opened vertically through the stricture. To do this, one makes an incision over the bulbar urethra under the scrotum to expose the urethra. But, instead of the extensive dissection required for excision and reconnection, now one simply opens the urethra through the narrowed portion. Buccal mucosa is then harvested from inside the cheek, and this tissue is then sewn onto the urethra thus increasing its diameter. The opened urethra is then closed over this repair, and the patient heals with a catheter in place for typically two weeks. Success rates for typical bulbar urethroplasties are greater than 90% long term.
Bulbar Urethroplasty
A: Typical 3cm bulbar urethral stricture. B: Appearance of same bulbar urethra after urethroplasty.
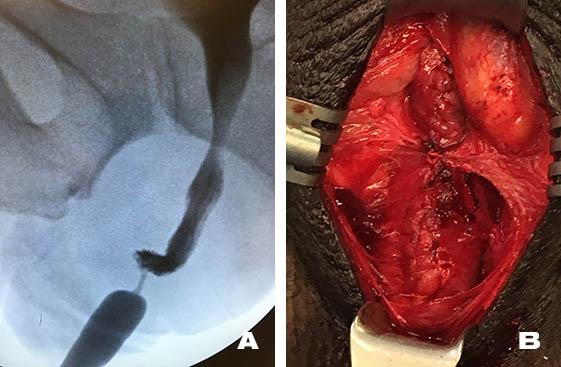
A bulbar urethroplasty can be done as an outpatient, but Dr. Engel commonly keeps such patients overnight in the hospital. Patients will be asked to gargle with an antiseptic four times a day for a few days if buccal mucosa has been harvested. The catheter will be removed if no leaks are demonstrated by an x-ray called a retrograde urethrogram approximately two weeks later.
Risks included scarring or pain in the mouth, recurrence of stricture, or leaking or infection around the site of graft placement or in the scrotum.





